The #1 eSignature Solution
Keep your business moving forward faster with the smarter AI-assisted eSignature

What you can do
Solve the problems that slow your agreements down with Docusign eSignature
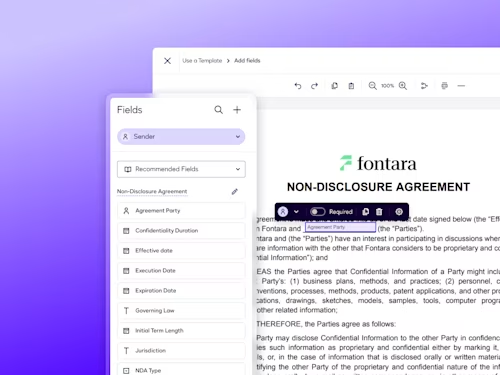
- Prepare and send agreements faster
AI detects your agreement type and auto-suggests the right fields, helping you get documents out the door with less manual work.
- Reach the right people, the first time
Pre-send verification confirms recipient details before your eSignature agreement goes out.
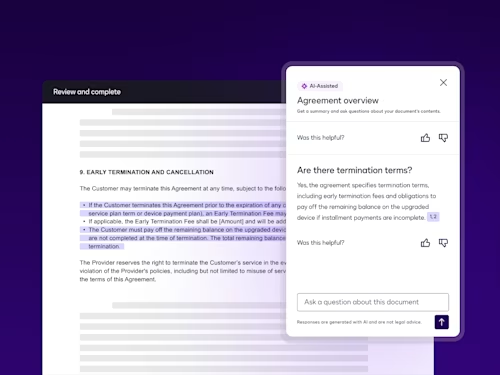
- Help readers understand and accelerate signing
AI-generated summaries and built-in Q&A give signers clarity faster so they can sign with confidence.
- Keep your workflows connected and error-free
Integrated automated flows keep your agreement data consistent and reduce rework across your tools.

Feature highlight
Reduce prep time with integrated document generation and eSignature
From automated redlining to instant compliance checks, we’ve built the tools to help you get to ‘signed’ faster.
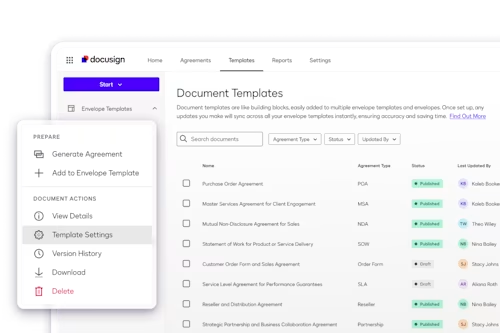
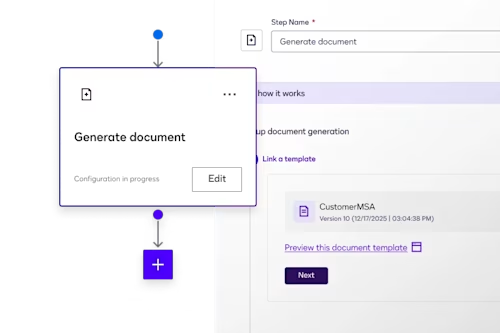
Document generation
Dynamically pull data from systems of record like Salesforce, and SAP to generate personalized agreements.
Secure, multi-channel delivery
Reach the right people on the right channel at the right time, with built-in verification.
eSignature for Enterprise
Enterprise-ready and compliance-tested
Create, commit, and manage every agreement faster without sacrificing compliance. Enterprise Pro combines eSignature with enterprise-grade authentication, policy controls, and reporting.
Advanced workflows for complex teams
Go beyond standard routing with agent and editor recipient types, conditional workflows, and shared access.
Built for strict compliance
Add advanced signer authentication, PDF/A archiving options, and specialized offerings for regulated environments.
Centralized admin for every account and user
Advanced admin packages with SSO, domain control, and organization-wide management so IT can manage users, policies, and integrations from one place.
Deeper data and integration options
Unlocks advanced data feeds and enterprise admin for integrations so you can flow eSignature activity into your analytics stack and manage connections.
Docusign Iris turns agreement insights into action with AI Agents that can help you close your agreement cycles faster
Docusign Iris turns agreement insights into action with AI Agents that can help you close your agreement cycles faster
Agreement detection
Scans your agreement to detect its type so you can see the most relevant fields faster.
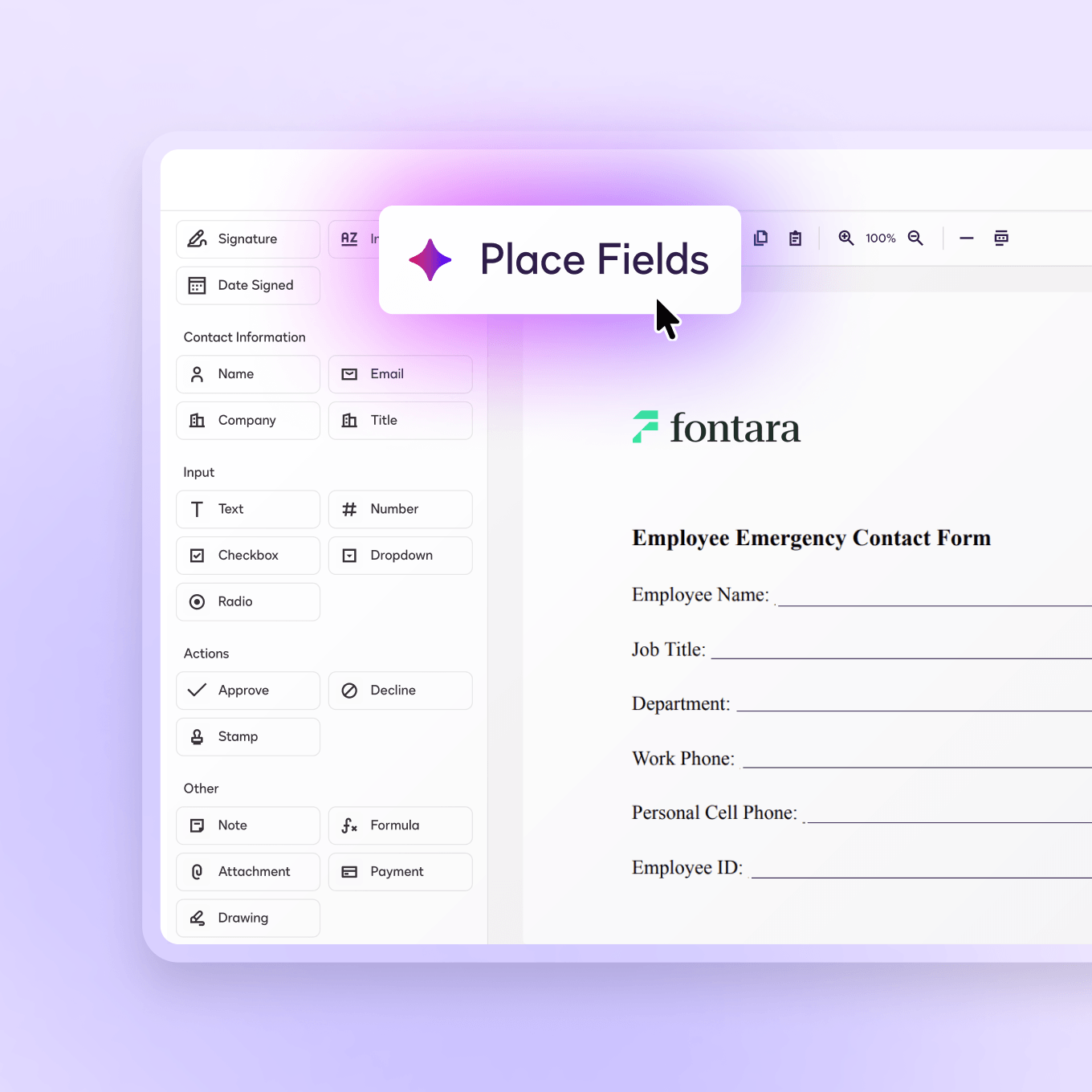
Field suggestions
Automatically identifies and helps place fields to speed up document preparation.
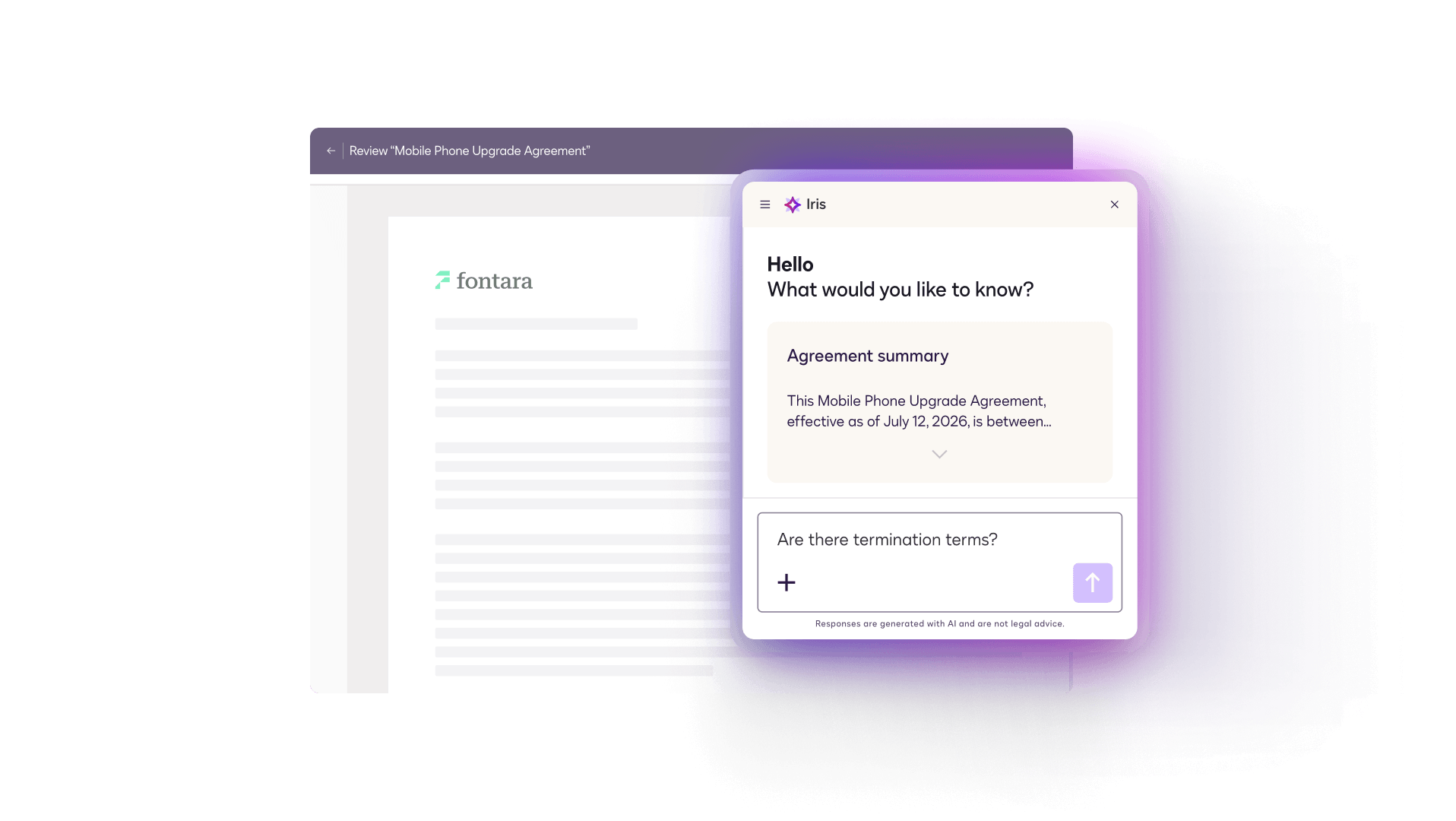
Agreement summaries and Q&A
Provides clear, AI-powered summaries and an instant Q&A tool to clarify complex details on the spot.
Get the clarity you need
Discover IrisCustomer success stories
Powering progress for 1.7 million customers
See how 1 billion people use Docusign solutions to accelerate the process of doing business, including startups and global enterprises.
Plans & Pricing
Find the right eSignature plan for your business
Personal
For individuals and sole proprietors with basic e-signature needs.
- Send 5 envelopes/month for signature
- Save time and standardize your agreements with reusable templates
- Stay in the tools you already use—expand your workflows with 900+ integrations
Standard
For small to medium teams that need to send, sign, and collaborate.
- Send a total of 100 envelopes/user/year
- Accelerate collaboration with shareable templates and real-time commenting
- Enhance customer trust with custom branding
Business Pro
For automating and optimizing agreements with advanced features.
- Send a total of 100 envelopes/user/year
- Collect data with mobile-friendly, interactive web forms
- Collect payments during the signing process
- Streamline attachment requests for signers
- Auto-calculate values with conditional logic
- Bulk-send envelopes to multiple signers
Explore related eSignature resources

Nearly 30% higher ROI with automated agreement workflows
Read the full Deloitte report that surveyed 1100 business leaders across 6 countries to uncover how agreement management can create real business value.
eSignature FAQs
An electronic signature is a catch-all term for any electronic process that indicates acceptance of an agreement or a record. The U.S. Federal ESIGN Act defines an “electronic signature” as “an electronic sound, symbol, or process, attached to or logically associated with a contract or other record and executed or adopted by a person with the intent to sign the record.”
The laws surrounding e-signatures enhance the credibility and trust of electronic records.
Electronic signatures are commonly used to sign offer letters, sales contracts, permission slips, rental/lease agreements, liability waivers, financial documents, and more. They are legally enforceable in most business and personal transactions worldwide. Learn more in our eSignature Legality Guide.
With Docusign eSignature, signing is always free. Recipients click a link to open the agreement on a device of their choice, such as a mobile phone, tablet, or computer. Tabs and simple instructions guide the user through the signing process, even adopting an electronic signature. The recipient clicks Finish to save the signed document.
The majority of commonplace agreements and forms can be signed electronically. Examples of documents that may be signed electronically include NDAs, purchase orders, vendor agreements, insurance claims, and hiring contracts.
The IAM platform can deliver more value to our existing customers by automating and connecting the steps before and after the signature, helping them address their end-to-end agreement workflows.
Below are some examples of the functionality available with Docusign IAM:
Tailored applications built for the unique needs of different lines of business and industries.
Modular capabilities and workflow designer let you build agreement process solutions that match your business needs in an easy-to-use, no-code environment.
Enhanced integrations and interoperability help seamlessly connect agreement processes with critical business systems, enabling agreement data to flow across Docusign and partner solutions.
A single, intelligent repository to centrally store, manage, and analyze agreements across the organization, unlocking data trapped in agreements to drive efficiencies, uncover opportunities to lower costs, and help reduce risk.
Yes, e-signatures are legally recognized around the world. In the U.S., the ESIGN Act, which was signed into law in 2000, grants legal recognition to electronic signatures and records if all parties to a contract choose to use electronic documents and to sign them electronically. Many foreign jurisdictions also recognize the legal effect and admissibility of electronic records. An electronic signature, like those supported by Docusign eSignature, is typically all that is needed to create a legally enforceable document. There are laws that demand certain requirements for e-signatures to be deemed legally enforceable. Using secure electronic signature software like eSignature can help you meet these security and compliance standards.
Read more about the legality of electronic signatures.
Get Started Today
eSignature supports agreements as flexible and dynamic as the way you run your business.